Hi All.
Following the ART conference, and some discussion relating to wet isolators and various 'techniques' for dealing with such issues, I thought I share our procedure.
I only have experience with Braun evolution lines that utilise three manometer connections, venous, arterial and pressure at dialyser inlet (for a standard HD treatment). This procedure only works if there is a bubble trap and spare locking luer fitting on the bubble trap. In the case of Braun lines the arterial line does not have a bubble trap so our policy would be to change the lines should this become wetted with blood. If either of the other luers becomes wet we ustilise the item below
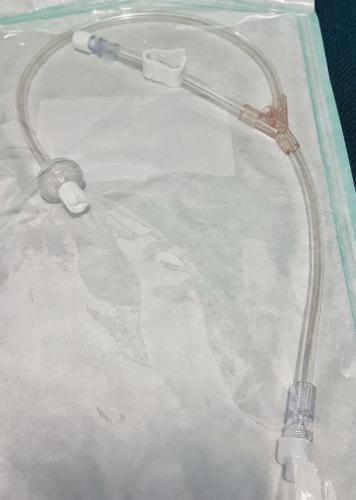
- The COP includes guidance to clamp existing wet isolator line and disconnect from equipment
- Attach new transducer protector y-connector above by securing locking luer to top of bubble trap and new isolator to machine.
- As per guidance, technologists are informed of wet isolator so that luer and internal filters/lines can be inspected post treatment.
- Yconnector provides spare connection for attachment of syringe as per original blood lines.
Hopefully useful for somebody out there